In OTC
Follow this topic
Bookmark
Record learning outcomes
There are an extraordinary number of things that could cause an allergic reaction. There are common allergens, such as foods, cosmetics, medicines and environmental substances like pollen (which causes hayfever), but an allergy can be triggered by anything that the body mistakenly identifies as a threat.
With so many potential irritants, pharmacy teams are likely to encounter allergic reactions frequently. It is therefore important that you are aware of different types of allergies and how to prevent, spot and treat them.
This is especially true since, according to the European Academy of Allergy & Clinical Immunology: “Allergy is the most common chronic disease in Europe. Up to 20 per cent of patients with allergies struggle daily with the fear of a possible asthma attack, anaphylactic shock, or even death from an allergic reaction.”
Understanding food allergies
Food allergies can range in severity, from causing digestive problems and discomfort to eczema, fainting and even anaphylaxis – a potentially life-threatening reaction that requires immediate medical attention.
Symptoms can occur within minutes to a couple of hours after consuming an allergen.
“The most common primary food allergies are caused by cow’s milk, eggs, peanuts, tree nuts, fish, crustaceans, soy and wheat. In children, allergies to cow’s milk, eggs and soy are the most common, with many childhood cases of these allergies being outgrown,” says Anne Biggs, deputy head of Clinical Services at Allergy UK.
“There is increasing clinical recognition of allergies to other legumes, such as peas, lentils, beans, and chickpeas, beyond the well-known allergies to peanuts and soy, although consistent UK data on this is limited.”
The first step to customers being able to prevent allergic reactions and knowing what to do if they experience one, is to get diagnosed – a task that is sometimes easier said than done.
“It can be difficult to know whether the signs and symptoms you or your child are experiencing are related to a food allergy because they can be commonly seen in other conditions,” says Anne.
“Allergic symptoms can be divided into those that happen within minutes of exposure (usually within 30 minutes) to the suspected food allergen – referred to as immediate or IgE mediated reactions – and those that happen several hours after exposure – often referred to as delayed or Non-IgE mediated reactions.
“The timing of symptoms can offer important clues as to whether the immune system is involved. Symptoms of an immediate IgE mediated allergy commonly affect the skin, causing rashes, reddening of the skin, hives, swelling and, in more severe cases, breathing difficulties.
Delayed reactions commonly affect the gastrointestinal system and include symptoms of vomiting, abdominal pain, diarrhoea, constipation and excessive wind.”
Allergy UK has a useful factsheet on allergy testing that customers can refer to. Testing can be a tricky process as there are various testing methods depending on the suspected allergen and/or clinical history of the person.
“It is important that IgE mediated allergy is recognised and diagnosed as soon as possible, as this is the type of allergy that has the potential risk of a severe allergic reaction,” says Anne.
Feeling the fever
Few pharmacy team members will need to be told about the prevalence of hayfever in the UK. The Government estimates that hayfever affects 10 to 15 per cent of children and 26 per cent of adults in the UK, and is becoming more common – with cases having trebled in the last 20 years.
On top of this, hayfever sufferers are being affected for longer periods of the year, as pollen seasons are changing due to climate change.
Some people develop hayfever as children, but it can impact customers for the first time as adults too.
“When someone suffers from hayfever, they are allergic to the pollen and spores that plants release into the air, often called allergic rhinitis, which affects an estimated 16 million people in the UK every spring and summer,” says Dr Roger Henderson, GP and spokesperson for Olbas.
“Many people ask whether hayfever is actually getting worse year by year. It isn’t that every single season is worse than the last, but overall, there is good evidence that pollen seasons in the UK are becoming longer and starting earlier.
“Climate change is a major factor, as warmer temperatures extend the growing season for plants and increase pollen production. In addition, air pollution can interact with pollen particles and make symptoms more severe, particularly in urban areas.”
While hayfever is not the only allergic reaction pharmacy teams will see at this time of year, Dr Henderson says it will be a main cause of symptoms for customers.
“This allergic reaction causes the all too familiar symptoms of hayfever – sneezing, a blocked nose and a sore throat,” he says.
Hayfever can also cause coughing, a runny nose, itchy, watery or red eyes, and an itchy mouth, throat, nose and ears. Some people may also experience a headache, feeling tired, loss of smell, and pain around the sides of the head and forehead.
It is not uncommon for customers to think they are coming down with a cold or the flu, as the symptoms are not dissimilar – but make sure to check how long customers have been struggling for as this may indicate hayfever.
“Prolonged sinus congestion due to hayfever may also increase the risk of developing sinusitis”
Treating hayfever
While hayfever is common and often thought of as a relatively low-maintenance, manageable condition, it can cause issues like disruption to sleep, which we know has a multitude of ripple effects.
One of these is impaired daytime concentration, leading some people to miss days of work or school.
There are plenty of self-care practices you can suggest to hayfever sufferers to hopefully avoid missing school, social activities and limit its interference in daily life.
“Although symptoms can be unpleasant and cause discomfort, there are practical steps pharmacy teams can provide to patients to help them manage symptoms,” says Dr Henderson. His top tips include:
- Stay indoors on days when the pollen count is high, to limit contact with allergens
- Keep doors and windows closed when the pollen count is high. Try to avoid outdoor areas where there’s more pollen, such as grassy parks, especially in the early morning, late afternoon and evening when the pollen count is highest
- Don’t mow the grass (and stay inside if it’s being mowed by someone else)
- Invest in a pair of wrap-around sunglasses to keep pollen out of the eyes
- Take a shower after going outside when the pollen count is high to wash off any lingering allergens
- Consider whether any house and garden plants trigger symptoms of hayfever and move them if necessary
- While drying washing outside is usually recommended, if the pollen count is high, pollen may get trapped in the fibres of clothes and bed linen
- Put petroleum jelly on the inside of nostrils to prevent pollen from entering the nasal passages.
Over-the-counter treatments can also be recommended, depending on the customer’s needs and preferences. Dr Henderson recommends decongestants in various forms to help alleviate symptoms.
“Decongestants can sometimes be very helpful in reducing the symptoms of nasal congestion,” he says. “Hayfever causes inflammation and swelling in the nasal passages, and decongestants help to reduce this swelling, helping people to breathe more easily.”
Decongestant nasal sprays containing the ingredients xylometazoline or oxymetazoline should, however, only be used for a short amount of time. This is to avoid rebound congestion from occurring when they are stopped.
“Decongestant nasal sprays provide quick relief by shrinking nasal tissue directly. They are very useful during the peak hayfever season when nasal congestion is at its worst, at bedtime to help reduce snoring or nasal blockage at night, and before going outside on high-pollen days,” says Dr Henderson.
“Because they treat symptoms rather than the underlying allergic reaction, you still need antihistamines or other allergy treatments.”
Antihistamines are available OTC and work by blocking the effects of histamine in the body – this chemical is released when the body detects something harmful (in this case, the allergen).
Antihistamines can be divided into two main types – drowsy and non-drowsy. Customers may need to undergo a trial and error period to see which type works best for them.
Generally, non-drowsy products containing ingredients such as cetirizine, loratadine, and fexofenadine are recommended for daytime use. Products with ingredients that are likely to cause drowsiness (e.g. chlorpheniramine, diphenhydramine) may be perfect for those whose symptoms disrupt their sleep.
If left untreated…
People with hayfever are at an increased risk of developing conditions such as asthma and/or eczema, if they do not already have them.
“Hayfever is a risk factor for the development of asthma and may contribute to poor asthma control and the worsening of asthma symptoms,” says Dr Henderson.
“Hayfever symptoms can also affect sleep, leading to fatigue. Prolonged sinus congestion due to hayfever may also increase the risk of developing sinusitis, and in children, hayfever is often a trigger for the development of middle ear infections called otitis media.”
Customers concerned about any of these symptoms should be referred to the pharmacist.

Itchy, red and/or watery eyes are a main symptom of hayfever.
“Allergic rhinitis affects an estimated 16 million people in the UK every spring and summer”
Chronic spontaneous urticaria
Although not technically caused by allergens, the skin condition chronic spontaneous urticaria (CSU) is caused by an immune response in the body which is similar to an allergic reaction.
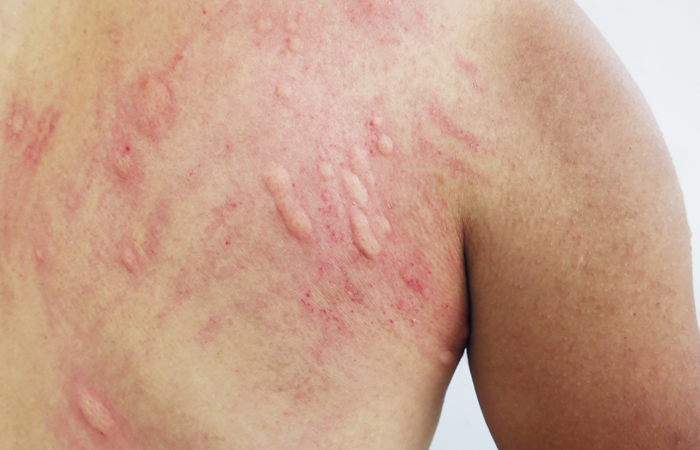
In those affected by CSU, mast cells that circulate in the blood release histamine, amongst other chemicals, into the skin’s tissue. This shows up as a red, itchy, raised rash that is sometimes described as hives or wheals.
“The rash can be tiny bumps or large raised patches of different shapes and sizes, and can affect any part of the body,” says Anne Biggs, deputy head of Clinical Services at Allergy UK.
“In our immune system, we all have mast cells, which circulate in the blood and are found in most tissues in the body. Mast cells help the immune system to reduce inflammation, fight infection and assist with wound healing and repair.
When you experience urticaria, mast cells in the immune system are activated due to a signal (trigger) and release chemicals, including histamine, into the skin’s tissue, causing the red, itchy raised rash,” Anne explains.
CSU can be especially frustrating because its triggers often cannot be avoided. “Research suggests that in about 50 per cent of people with CSU, the cause of their CSU is autoimmune.
This is when the body mistakes its own cells as harmful and so activates cells including mast cells which then cause the symptoms of urticaria,” says Anne.
To help customers, she suggests that pharmacy teams recommend the following tips:
- Soothe the skin. Applying cream-based or light emollients with antipruritic (anti-itch) ingredients such as lauromacrogols or menthol in aqueous cream can help to reduce itch and discomfort
- Avoid using perfumed or scented emollients, toiletries, cosmetics or bathing products. This can cause more irritation to the skin
- Apply an ice pack. This can often calm the itch sensation. A cool bath can also help. However, both should be avoided if cold temperatures affect the person’s urticaria
- Try to avoid scratching. Scratching releases more itch chemicals (histamine) and will make the itch worse
- Wear loose, light clothing. This helps to reduce itch and make the person feel more comfortable
- Try to relax. Reduce stress and avoid stimulants. In some people, avoiding alcohol, recreational drugs, caffeine and extremes of temperature can help to reduce symptoms
- Avoid certain medications if possible. Aspirin, non-steroidal anti-inflammatory (NSAIDs), opiates such as codeine and ACE inhibitors can make the symptoms of CSU worse in some individuals. Customers should seek medical advice before stopping them, however.
The first line treatment for CSU is a prescribed non-sedating antihistamine, so if customers are consistently struggling, they should be referred for diagnosis and a prescription if appropriate.